In April 1979, Raymond Wheeler went before a U.S. Senate subcommittee and explained that the federal government had achieved something barely imaginable a decade earlier.
Wheeler, a North Carolina doctor and one of the unsung heroes of the Civil Rights Movement, had traveled the United States in the late 1960s documenting pervasive hunger and malnutrition among the country’s poor. In Texas his team discovered children who suffered from rickets, a form of bow-leggedness caused by vitamin D deficiency; in Mississippi they visited starving families denied federal food aid by local political bosses.
Their report became the basis of a shocking 1968 TV documentary, Hunger in America. Middle-class viewers were appalled by the images they saw: tiny, underfed babies, hovering near death in hospital emergency wards; a hungry Texas boy who survived mostly on beans and could not afford his school’s lunch; children of Virginia tenant farmers whose unvaried potato diet left them with “a hollow, lifeless look,” in their doctor’s words.
Within a few years of the broadcast, however, such horrors had largely been vanquished.
Wheeler told senators that severe hunger had been virtually eliminated in the nation’s rural areas and urban slums. “Everywhere we looked in 1967 we found hungry children suffering the diseases that malnutrition cause. Now, in those same areas, there is nowhere the same evidence of gross malnutrition we saw then,” he reported.
In many parts of the country infant mortality had fallen by a third. Malnutrition-related deaths had been halved. Researchers attributed much of the improvement to major expansions of federal food stamp and school meal programs, as well the Head Start childcare program.
The expansion of these programs represented a triumph for the anti-hunger movement of the late 1960s. Years of intense activism had led President Richard Nixon to hold an unprecedented White House Conference on Food, Nutrition, and Health in 1969, where nutritionists and other experts recommended the boost in federal assistance and a host of other measures to improve the nation’s food system.
Yet Wheeler and other activists were hardly celebrating. As he told the senators in 1979, aid still hadn’t reached more than 60% of the people who needed it. The conference participants had recommended creation of a basic income program to address the poverty at the root of chronic hunger, but Nixon balked at the high cost and Congress never followed through. The government also left mostly unaddressed the growing problem of obesity and diet-related diseases, which developed into a national crisis in the ensuing decades.

Health advocates and nutritionists prodded successive administrations to again revamp the country’s food policies, but with mixed success. Startling images of need during COVID-19 lockdowns and protests for racial justice finally jolted officials into action. In May, President Biden announced a new White House Conference on Hunger, Nutrition, and Health to be held September 28.
As in 1969, reforms to food stamp (now called SNAP) and school lunch programs are on the docket. But this time around scientists and advocates are also promoting dozens of social, economic, and regulatory proposals to improve the quality of the nation’s diet. They want doctors to prescribe vegetables to their patients, government to tax sugar-sweetened beverages, and companies to put warning labels on junk foods.
Comprehensively changing a society’s eating habits is incredibly difficult, they say. Only by pursuing multiple approaches at once, including controversial new laws and regulations, do they have any hope of making a real difference.
“Politically difficult? Of course. Politically impossible? I do not think so,” wrote Marion Nestle, a well-known professor of nutrition and author of food industry exposés, in a recent editorial. “Unless we keep trying to intervene—and continue to examine the results of our attempts—we will be settling for the normalization of overweight and the personal and societal costs of its health consequences.”
Experts and Agitators
Nutritionists seeking to reverse the obesity epidemic are following in the footsteps of earlier scientists who sought cures for other diet-related diseases, sometimes in the face of apathy or outright hostility.
One such pioneer was Polish American biochemist Casimir Funk, who in 1912 formulated the idea of vitamins, or nutritional molecules that are essential for life. He proved that a deficiency of one such substance, thiamine, caused beriberi, and proposed that vitamins could prevent other conditions, such as rickets, scurvy, and celiac disease.
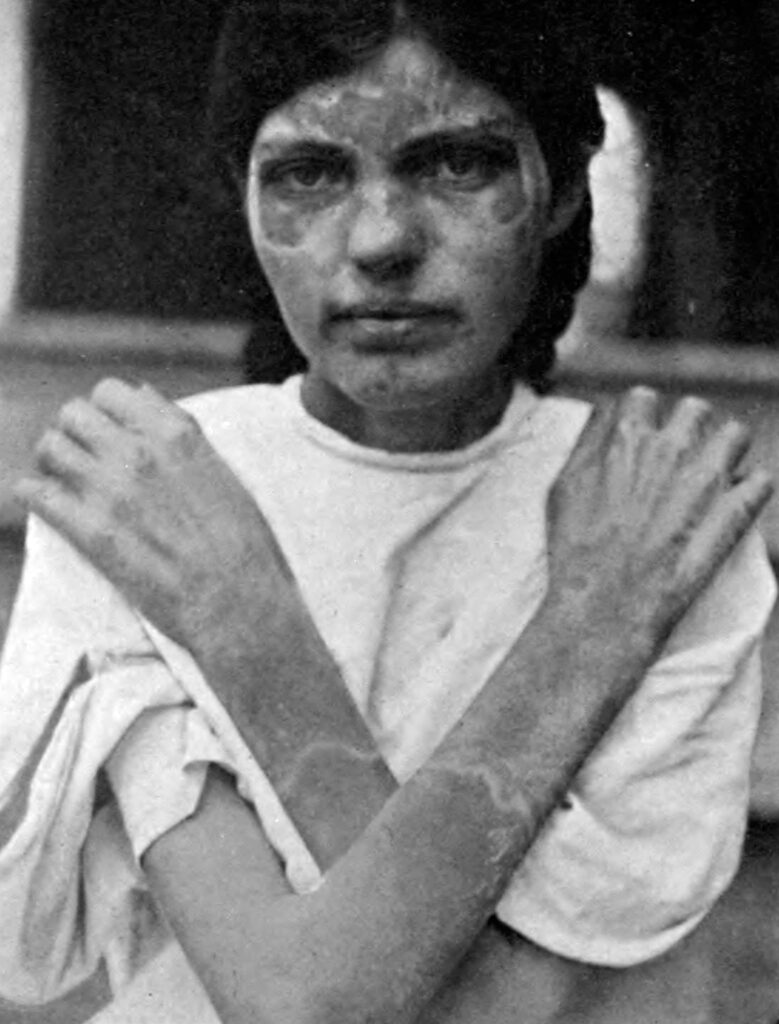
Funk came close to identifying the deficiency that caused pellagra, but his work received little attention despite the desperate need for a cure. At the time, Southern states were struggling with an epidemic of the mysterious disease, which sickened hundreds of thousands of people and killed 7,000 a year for several decades. In 1909 a National Conference on Pellagra was convened to study the problem. The clear association with poverty and poor diet was embarrassing to Southerners, who preferred to believe it was caused by an infectious agent. Researchers were attacked for bringing attention to the disease.
A few years later physician Joseph Goldberger showed that pellagra was associated with the region’s heavily corn-based diet, but when he sought federal funding to continue his research, he was roundly criticized; one South Carolina congressman responded by calling reports of widespread malnutrition in the state an “utter absurdity.”
In the late 1930s biochemist Conrad Elvehjem and other researchers finally demonstrated that niacin deficiency caused pellagra. States began legislating vitamin supplementation of common foods, and as a result pellagra and several other nutritional deficiency syndromes were virtually eliminated after 1940.
This apparent progress helps explain people’s shock a generation later, when Raymond Wheeler and other doctors revealed that diet-related diseases continued to rage across the South.
The problem now was a sheer lack of food rather than ignorance of biology. Investigators found that local political bosses were withholding surplus commodities to control destitute families, as journalist Nick Kotz recounted in his 1969 book, Let Them Eat Promises. In Mississippi and Texas, food aid was stopped in the spring to force workers to accept farm work at “near-starvation wages.” In Greenwood, Mississippi, benefits were cut off to punish Black people leading a voter registration drive. Many counties were switching from food giveaways to food stamps, which provided a discount on groceries but still had to be purchased, putting them out of reach for the poorest households.
During Senate testimony, civil rights attorney Marian Wright challenged members of a subcommittee on poverty to come see these injustices for themselves. Senators Robert Kennedy and Joseph Clark took Wright up on her invitation. After visiting starving families in the Mississippi Delta, they returned to Washington to demand emergency federal aid and a cut in food stamp prices. President Johnson refused to support the needed spending, and Southern legislators adamantly opposed anything that smacked of welfare, especially for their poor Black constituents. “When you start giving people something for nothing. . . I wonder if you don’t destroy character more than you might improve nutrition,” Mississippi Congressman Jamie Whitten said at one hearing.

But the larger anti-hunger movement gradually rolled over the objectors. CBS broadcast Hunger in America, 3,000 protesters from the Poor People’s Campaign camped out on the Washington Mall, and a 10-state National Nutritional Survey ordered by Congress put hard numbers behind the crisis. The newly elected Nixon decided to seize leadership of the issue from his political rivals. He gave a speech vowing to eliminate hunger once and for all and asked scientist Jean Mayer to set up a conference that would provide authoritative recommendations, while assuaging civil rights activists and enlisting help from the private sector and social service organizations.
Mayer, a leading researcher on the biology of hunger, was a prominent lobbyist for increased food aid. Other top scientists led the conference’s panels, including Mark Hegsted, who had established the link between saturated fats and increased dietary cholesterol; Ancel Keys, an expert on the effects of diet on heart disease; and Charles Upton Lowe, leader of the first-ever national nutrition survey of young children. Mayer brought in executives from Campbell Soup, Monsanto, and Pepsi-Cola to weigh in on food production trends, nutrition standards for high-tech, “simulated” foods, and food safety. The conference invited anti-poverty activists, consumer advocates, and poor people from around the country to weigh in.

The three-day event in early December 1969 was a largely sober-minded but occasionally contentious affair, with competing imperatives to at once give Nixon political advantage and press him for societal change. A smattering of activists loudly demanded huge new outlays of federal funds, while most of the 3,000 attendees—nutritionists, food manufacturers, representatives of consumer and community groups—discussed dietary needs and policy changes.
“These people were not rabble-rousers, confrontation-minded characters, hippies, yippies, or militants. They would have passed for any PTA meeting,” reported a correspondent for the Christian Science Monitor, who was annoyed by the noisy activists. “A majority seemed to have a Ph.D., or an M.D., or a D.D.S., or to be a professor, or chairman, or director of this or that organization; or a consultant, a government official, a researchist, or a nutritionist.”
“Nobody who was a power in nutrition said ‘no’ to going to that conference and working really hard to get it done,” nutritionist Jeanne Goldberg recalled in a recent interview. Goldberg was a young dietitian working for the Massachusetts Department of Public Health when she was enlisted to work on pregnancy and child nutrition issues for the conference. She later worked closely with Mayer, earned a PhD, and researched obesity and chronic disease prevention. “There was an excitement that things were really going to get done. And a lot of things did.”
The three-day event in early December 1969 was a largely sober-minded but occasionally contentious affair, with competing imperatives to at once give Nixon political advantage and press him for societal change.
At the time, the tensions among the conferees made the most news. Technocratic responses to malnutrition clashed with demands for long-term solutions to poverty. Several panels endorsed a proposal to give families a $5,500 basic income, which far exceeded the $1,600 per family Nixon was offering. When a member of a key panel on “systems of food delivery and of money for food” tried to explain the high cost—$70 to $80 billion a year—an anti-poverty activist shouted him down.
“What you’re doing is filibustering,” the man yelled. “You don’t know what a roach is. You don’t know what a rat is. Why don’t you shut up and let us talk?”
Mayer labored to craft a compromise. He finally got Nixon to agree to expand food programs to hundreds of counties that still lacked them, speed up an increase in food stamp benefits, and meet with activist leaders. That allowed the president to declare the event a success, although many conference participants found his concessions inadequate.

All told, the panels delivered 1,800 recommendations. Remarkably, an estimated 1,650 were rolled out within two years. The government expanded access to food stamps and to free breakfasts and lunches at school and launched the WIC nutrition program to address malnutrition among poor pregnant women and infants. The FDA began requiring nutrition and ingredient labeling of certain products and established the Generally Recognized As Safe ingredient classification, eliminating some potentially harmful additives from foods.
Federal scientists created the Dietary Guidelines for Americans, which translated nutrition science into clear guidance for the public. Overall, Americans became much more nutritionally aware, consumed less saturated fat, and had better options at the supermarket, including reduced-salt foods and low-fat milk.
The basic income plan never came to fruition, however, even at the lower amount Nixon had proposed.
Getting Congress’s Attention
More than 50 years later, economic hardship remains a stubborn obstacle to the eradication of hunger. The country’s poverty rate is 11.4%, down a bit from the late 1960s, but inequality has widened dramatically: the top 10% of Americans now hold nearly 70% of U.S. wealth, and the bottom 50% own just 2.5%.
In 2020, 11.8% of the population, or more than 38 million people, lived in households that struggled with food insecurity, a 9% jump from the previous year. About 4% of Americans, or roughly 13 million people, regularly skipped meals or ate less because they could not afford food.
That deprivation became starkly clear when the pandemic froze the economy. Despite federal stimulus checks, child tax credits, and an emergency SNAP expansion, many families were forced to turn to food banks for the first time. Images of miles-long lines of cars, their occupants waiting for hours to pick up a box of groceries, became a staple of daily news reports.
“When you think about food as a system, a lot of the components have been really in crisis, or the crisis has been exacerbated, the past few years,” said Emily Broad Leib, director of Harvard’s Food Law and Policy Clinic. “The COVID pandemic really threatened food security and led to a new acknowledgment and political will around hunger. Not that dissimilarly from the original White House conference in 1969, there’s been this discovery of hunger and how big of an issue it is.”
And like in the late 1960s, the country has seen a resurgent movement for racial justice, heightening calls for a fairer food system that provides not only sustenance but also nutrition security and good health for people of color. In his announcement of the conference, Biden noted the higher incidence of diet-related disease among Blacks, Hispanics, and Native Americans, as well as rural families and low-income households generally. Nearly 22% of Black households and 17% of Hispanic households are food insecure, compared to 7% of whites.
Like in the late 1960s, the country has seen a resurgent movement for racial justice, heightening calls for a fairer food system that provides not only sustenance but also nutrition security and good health for people of color.
Scrutinizing the country’s existing food programs is a conference priority, said Dan Glickman, the former Secretary of Agriculture in the Clinton administration. He’s a co-chair of a task force advising the White House organizers, along with Tufts University cardiologist Dariush Mozaffarian and other dignitaries.
“How are our federal feeding programs dealing with all the challenges we have, the higher degrees of food insecurity and poverty in some areas?” Glickman said. The conference will examine “these programs to make sure that they’re adequately funded, and how we get information to people so they take advantage of them.”
Proponents have plenty of ideas. Biden has proposed spending tens of billions to expand free school lunches and summer meals, while policy groups, such as the Center for Science in the Public Interest, say the conference should rewrite SNAP guidelines to permanently increase the benefit. These groups also are agitating to end bans on SNAP benefits for people with drug convictions, repeal work requirements, extend SNAP to Puerto Rico, and get more stores and online vendors into the program.

The fate of these changes rests in part on the Farm Bill, a perennially controversial law that covers a huge swath of food- and agriculture-related activity. When it comes up for reauthorization in 2023, some conservative congressmen may call for budget cuts and new eligibility restrictions for food programs, which account for three-quarters of its price tag. Various advocacy groups want to see more investment in sustainable agriculture, small farms, land conservation, and climate change mitigation. Others criticize the billions the USDA spends annually to subsidize large agribusiness companies, especially for cultivation of corn, soybean, and wheat, the top commodity crops.
“Part of the idea is to chart a course for some priorities,” Leib said. “Congress is very divided and may be likely to stay that way. So one question is, what are [the conferees] going to recommend? And which of those recommendations will have the political support to move forward?”
While expanding SNAP and school lunch programs is relatively straightforward, if expensive, using policy to improve diets is vastly more complicated.
Even the 1969 conference panelists recognized high incidence of obesity in the United States and associated increases in diabetes, hypertension, pulmonary dysfunction, and “social disability.” They recommended more public education and physical activity, less fat intake, and a guaranteed income for all Americans, “since it is very difficult or impossible to construct nutritious diets for the prevention and treatment of obesity and other illnesses from foods now available to the disadvantaged.”
Decades of persistent poverty and poor nutrition have greatly amplified the problem. When the White House made another push to improve nutrition with First Lady Michelle Obama’s Let’s Move! campaign in 2010, the focus was not hunger, but childhood obesity. By the time the pandemic struck, almost one in five children was obese, up from 5% in 1969.
About three-quarters of American adults are now considered overweight, and a staggering 42% are obese, up from 13% in the 1960s. Diabetes, once a rare disease, affects more than 1 in 10 people today. Meanwhile, obesity significantly increases risk of severe illness, hospitalization, and death from COVID-19. All of these harms are more common among Blacks and Hispanics.
About three-quarters of American adults are now considered overweight, and a staggering 42% are obese.
Diabetes now costs more than $327 billion annually in health care spending and lost productivity. Adding in cardiovascular disease and other conditions, the cost of obesity has been estimated at $1.72 trillion a year. Mozaffarian, who is Jean Mayer Professor of Nutrition at Tufts and one of the main advocates for holding a new conference, frequently cites these costs as arguments for speedy policy reform.
“This is absolutely not sustainable,” he said at a Senate hearing last November. “Rising healthcare costs are squeezing every other priority out of the federal budget, state budgets, and the balance sheets of U.S. businesses. We have to get these health care costs under control, and we’re absolutely not going to do it until we address the top cause, which is poor nutrition.”
Mozaffarian offers a long list of steps to reverse the obesity trend, which he calls “Food Is Medicine” solutions. These include doctors writing produce prescriptions for people with low incomes or diet-related health problems, restrictions on purchasing unhealthy foods with SNAP, and improved product labeling. Food companies could be encouraged to voluntarily reduce sodium, sugar, and trans fats in their products, or the FDA could compel them to do so. The government could subsidize healthy foods, such as produce, beans, whole grains, and fish. Mozaffarian and his task force co-chairs are also calling for national nutrition surveys, creation of a National Institute of Nutrition, and a “moonshot” research program, among many other measures.
But Nestle and others say there are powerful reasons why the government has not already launched a comprehensive battle against obesity. “Nobody is going to do anything about it,” she argued in an interview. Reform “is very hard to do and it means taking on the food industry.”
Food manufacturers are under intense pressure from shareholders to maximize their profits in a cutthroat market, she said. They painstakingly cater to consumers, who are attracted to larger portion sizes and what she calls “ultra-processed foods”—calorie-dense products such as candy, soft drinks, cereals, pizza, chips, and chicken nuggets. For decades food chemists have battled to make their companies’ products the most irresistible in the snack aisle, packing them with ever more sugar, salt, fat, artificial flavors, and stabilizers.

As a result of these innovations, along with a decrease in home cooking and other lifestyle changes, Americans simply eat way too much, especially junk food, Nestle said. The country produces enough food to supply 4,000 calories per person per day, or roughly twice as much as dietary guidelines call for—and companies need to sell all that product.
Individual interventions, such as improving calorie labeling or opening a supermarket in a low-income neighborhood, tend to produce small effects. But Nestle says programs that integrate multiple interventions have shown more promise.
She notes that after Chinese researchers spent a year teaching schoolchildren and their families about exercise and junk food and restricting sales of unhealthy products, the students’ obesity rate fell 27%. Nestle also praised the Blue Zones Project, which works with cities to apply multiple interventions at once, such as walkable streets, healthier restaurant food, and education programs in stores. In a 20-year study of participating California cities, one project succeeded in significantly reducing obesity and cardiovascular risk factors, such as hypertension, compared to the state as a whole.
“How do you create a food environment that encourages healthy eating and makes healthy eating pleasurable, desirable, affordable, accessible, all of those things? These are political questions,” Nestle said.
Coaxing people to change their lifestyles is difficult but not inconceivable. With the stakes so high, Nestle said that, despite her doubts, she is eager to see if this year’s conference can move the needle in a positive direction.
“Everybody wants to go. Invited or not, I want to go,” she said. “It’s a historic event.”






